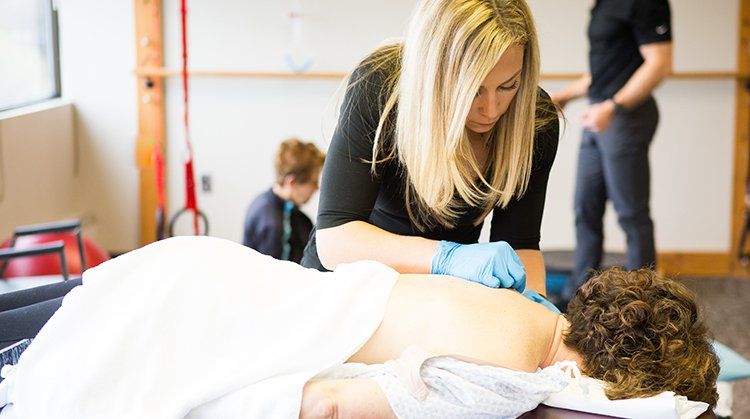






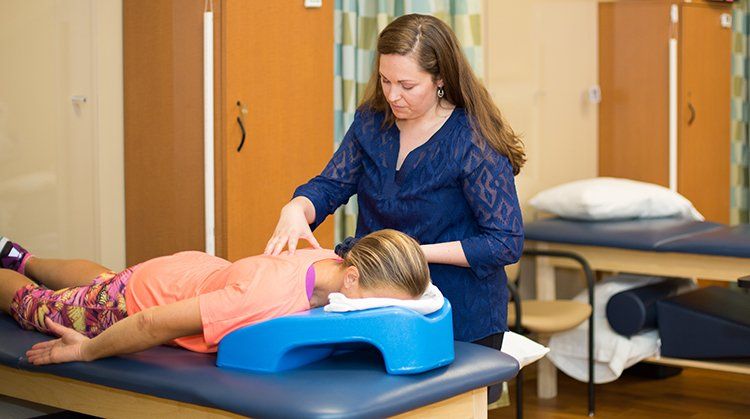

"Arthritis" is a term used to describe inflammation of the joints. Osteoarthritis (OA) is the most common form of arthritis and usually is caused by the deterioration of a joint. Typically, the weight-bearing joints are affected, with the knee and the hip being the most common.
An estimated 27 million Americans have some form of OA. According to the Centers for Disease Control and Prevention, 1 in 2 people in the United States may develop knee OA by age 85, and 1 in 4 may develop hip OA in their lifetime. Until age 50, men and women are equally affected by OA; after age 50, women are affected more than men. Over their lifetimes, 21% of overweight and 31% of obese adults are diagnosed with arthritis.
OA affects daily activity and is the most common cause of disability in the US adult population. Although OA does not always require surgery, such as a joint replacement, it has been estimated that the use of total joint replacement in the United States will increase 174% for hips and 673% for knees by 2030.
Physical therapists can help patients understand OA and its complications, and provide treatments to lessen pain and improve movement. Additionally, physical therapists can provide information about healthy lifestyle choices and obesity education. This is important because some research shows that weight loss can reduce the chance of getting OA. One study showed that an 11-pound weight loss reduced the risk of OA in women.
Your bones are connected at joints such as the hip and knee. A rubbery substance called cartilage coats the bones at these joints and helps reduce friction when you move. A protective oily substance called synovial fluid is also contained within the joint, helping to ease movement. When these protective coverings break down, the bones begin to rub together during movement. This can cause pain, and the process itself can lead to more damage in the remaining cartilage and the bones themselves.
The cause of OA is unknown. Current research points to aging as the main cause. Factors that may increase your risk for OA include:
Typically, OA causes pain and stiffness in the joint. Common symptoms include:
Caution: Swelling and warmth around the joint is not usually seen with OA and may indicate a different condition or signs of an inflammation. Please consult with your doctor if you have swelling, redness, and warmth in the joint.
Osteoarthritis is typically diagnosed by your doctor using an x-ray, but there are signs that may lead your physical therapist to suspect you have OA. Joint stiffness, difficulty moving, joint creaking or cracking, and pain that is relieved with rest are typical symptoms.
Your physical therapist can effectively treat OA. Depending on how severe the OA is, physical therapy may help you avoid surgery. Although the symptoms and progression of OA are different for each person, starting an individualized exercise program and addressing risk factors can help relieve your symptoms and slow the condition's advance. Here are a few ways your physical therapist can help:
In cases of severe OA that are not helped by physical therapy alone, surgery, such as a knee or hip replacement, may be necessary. Your physical therapist will refer you to an orthopedic surgeon to discuss the possibility of surgery.
The best way to prevent or slow the onset of OA is to choose a healthy lifestyle, avoid obesity, and participate in regular exercise.
The American Physical Therapy Association (APTA) believes that consumers should have access to information that could help them make health care decisions and also prepare them for their visit with their health care provider.
The following articles provide some of the best scientific evidence related to physical therapy treatment of hip osteoarthritis and hip replacement. The articles report recent research and give an overview of the standards of practice both in the United States and internationally. The article titles are linked either to a PubMed* abstract of the article or to free full text, so that you can read it or print out a copy to bring with you to your health care provider.
Centers for Disease Control and Prevention. Prevalence of doctor-diagnosed arthritis and arthritis-attributable activity limitation: United States, 2007-2009. Published October 8, 2010. Accessed March 11, 2013. Free Article .
Murphy LB, Helmick CG, Schwartz TA, et al. One in four people may develop symptomatic hip osteoarthritis in his or her lifetime. Osteoarthritis Cartilage. 2010;18:1372–1379. Free Article .
Cibulka MT, White DM, Woehrle J, et al. Hip pain and mobility deficits—hip osteoarthritis: clinical practice guidelines linked to the international classification of functioning, disability, and health from the Orthopaedic Section of the American Physical Therapy Association. J Orthop Sports Phys Ther. 2009;39:A1–A25. Free Article .
Murphy L, Schwartz TA, Helmick CG, et al. Lifetime risk of symptomatic knee osteoarthritis. Arthritis Rheum. 2008;59:1207–1213. Free Article .
Kurtz S, Ong K, Lau E, et al. Projections of primary and revision hip and knee arthroplasty in the United States from 2005 to 2030. J Bone Joint Surg Am. 2007;89:780–785. Article Summary in PubMed .
Deyle GD, Allison SC, Matekel RL, et al. Physical therapy treatment effectiveness for osteoarthritis of the knee: a randomized comparison of supervised clinical exercise and manual therapy procedures versus a home exercise program. Phys Ther. 2005;85:1301–1317. Free Article .
*PubMed is a free online resource developed by the National Center for Biotechnology Information (NCBI). PubMed contains millions of citations to biomedical literature, including citations in the National Library of Medicine’s MEDLINE database.
Authored by Christopher Bise, PT, MS, DPT. Reviewed by the MoveForwardPT.com editorial board .








